February 01, 2026
©L’ORIENT OFFICIAL / FILED UNDER: skincare 101
Understanding Confluent and Reticulated Papillomatosis (CARP) as a Hidden Cause
Dark underarms are one of the most common concerns I see in clinic. But here is the truth many people never hear:
Dark underarms are not a diagnosis. They are a symptom.
When patients tell me they have tried every exfoliant, brightening cream, and deodorant on the market with no improvement, it raises an important clinical question:
What is actually causing the pigmentation?
There are multiple medical and skin conditions that can present as “dark underarms,” including:
Post-inflammatory hyperpigmentation (from shaving, waxing, friction, or eczema)
Acanthosis nigricans (linked to insulin resistance and hormonal changes
Fungal or bacterial overgrowth
Contact dermatitis from deodorants
Genetic pigment patterns
And a lesser-known but important condition: Confluent and Reticulated Papillomatosis (CARP)
What is CARP?
Confluent and Reticulated Papillomatosis (CARP) is a disorder of abnormal skin cell turnover and keratinisation.
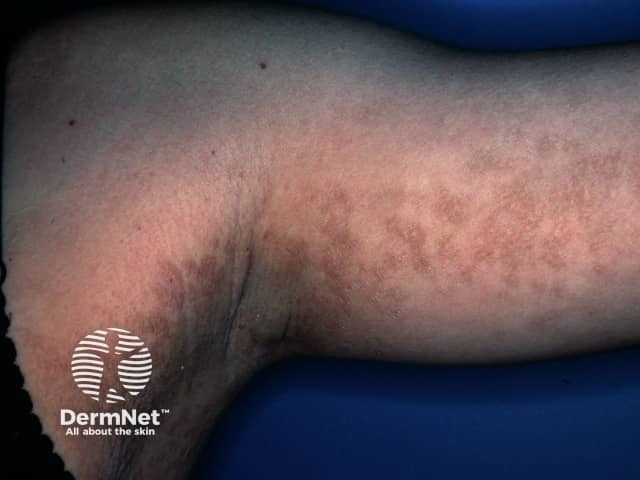 Image courtesy of DermNet, link to original source here
Image courtesy of DermNet, link to original source here
Although it occurs across all ethnicities, studies suggest it is more prevalent in Caucasian populations and typically affects adolescents and young adults between ages 8 and 32.
It often begins on the chest and upper back and can spread to:
Neck
Underarms (axilla)
Shoulders
Upper arms
Groin and pubic region
Skin folds
Clinically, it appears as brown or grey, velvety, slightly scaly patches with a reticulated (net-like) pattern. Because of its colour and location, it is frequently mistaken for fungal infections or simple hyperpigmentation.
What Scientists See Under the Microscope
When CARP-affected skin is examined using electron microscopy (a very high-powered microscope), several consistent abnormalities appear.
1. Disordered skin maturation
Normally, skin cells move upward through the epidermis in a highly organised way, eventually forming the stratum corneum, our protective barrier.
In CARP:
Skin cells mature too quickly and incorrectly
They become stuck between layers
The normal “brick wall” structure of the skin barrier is disrupted
The surface becomes thickened and rough
This is described as hyperproliferative and disordered keratinisation.
2. Excess lamellar granules
Lamellar granules are tiny packets inside skin cells that release fats and lipids needed to build a healthy barrier.
In CARP:
There is an increased number of these granules
This suggests the skin is trying to compensate for barrier dysfunction
But the process is uncoordinated and ineffective
The result is abnormal barrier formation rather than repair.
3. Increased melanosomes in the outer layers
Melanosomes are the packets that carry melanin (pigment).
In CARP:
More melanosomes are trapped in the outer dead skin layers
This explains why CARP looks brown or grey rather than just scaly
Pigment is retained because cells are not shedding normally
So this is not simply “extra melanin production,” but melanin being trapped in abnormal skin layers.
4. Transitional cells stuck between layers
Researchers found increased numbers of “transitional cells” between the granular layer and the outer horny layer of skin.
This means:
Cells are getting stuck halfway through maturation
The skin never completes its normal renewal cycle
Leading to thickened, velvety plaques
5. Genetic stress signals in some patients
In families with CARP, scientists found increased expression of keratin 16, a stress-response keratin.
Keratin 16 is usually seen in:
Psoriasis
Wound healing
Inflamed or rapidly turning-over skin
This suggests that in some individuals, CARP may have a genetic predisposition affecting how skin responds to stress and inflammation.
Infection as a Possible Trigger
CARP was historically thought to be triggered by infection because it responds well to antibiotics.
The leading candidate organism is Dietzia papillomatosis, a gram-positive actinomycete.
Antibiotics likely work through:
Anti-inflammatory effects
Altering skin microbiome balance
Modulating keratinisation pathways
This is why antifungals alone often fail.
How CARP is Diagnosed
Diagnosis is usually clinical and based on:
Typical appearance and location
Lack of fungal elements on potassium hydroxide (KOH) testing
Exclusion of tinea versicolor
Differentiation from acanthosis nigricans
Histologically, CARP shares features with acanthosis nigricans:
Hyperkeratosis
Papillomatosis
Mild superficial inflammation
However, follicular plugging can help distinguish CARP from acanthosis nigricans.
Treatment Approach
First-line treatment:
Oral minocycline
Second-line:
Macrolide antibiotics (if minocycline not tolerated)
Other options:
Topical retinoids
Vitamin D analogues
Tacrolimus
Alternative antibiotics
Oral isotretinoin for resistant cases
For itch or inflammation:
Short courses of topical corticosteroids
Tacrolimus or pimecrolimus for long-term control
Long-term steroid use must be monitored due to risk of skin thinning and pigment changes.
Why This Matters for Dark Underarms
If someone has CARP affecting the underarms, OTC exfoliating acids, and antifungals alone will not resolve the problem.
Because the issue is:
Abnormal keratinisation
Barrier dysfunction
Trapped pigment
Inflammatory signalling
It requires medical intervention, first.
Usually this means starting with oral antibiotics, a single course of this is reported to lead to remission for up to 2 years in many cases. To enhance pigmentary return to baseline, a product like ÈCLAIR can be utilised safely alongside oral therapy to expedite clearance of pigmentation and normalise the barrier architecture here without stripping the skin.
Both prescription antibiotics are needed however, for optimal results!
And if brightening stalls or is slow, besoke prescription topicals like our coming NIGHT SHIFT range can do the final trick.








